NICE recommends Chronic Primary Pain Treatments: Acupuncture and talking therapies; CBT and ACT
You may have seen the recent press stories about Acupuncture, and two specific talking therapies; Cognitive Behavioural Therapy (CBT); and Acceptance and Commitment Therapy (ACT), being among the main suggested treatments by NICE for the management of chronic primary pain. This was in the latest NICE draft guidelines, August 2020.

This is instead of prescribing painkillers, which are no longer recommended in this condition, with acupuncture, CBT and ACT being assessed by NICE, as being more effective than painkillers.
This an interesting development, so we decided to explain a bit more about it, and the treatments themselves which are all offered here, at Bedford Consulting Rooms.
Specific pages about the treatments tell about what they are, and how they work, as well as linking to the practitioners who practise them here:
CBT – Cognitive Behavioural Therapy
ACT – Acceptance and Commitment Therapy
What is NICE?
NICE (National Institute for Clinical Excellence) is the advisory body to the NHS, a committee which appraises scientific evidence and costing aspects of available treatment choices for certain conditions; from this, NICE produces guidelines which are used by NHS doctors and clinicians in their decision-making regarding prescribing, referrals to consultants or surgery and treatment recommendation.
What is chronic primary pain?
Ongoing, or persistent pain which endures over a long period of time, but that which is not explainable by another disease state or cause. Chronic pain can impact greatly on the daily life on patients and their families, many of whom cannot work, and with half of them being diagnosed with depression alongside the pain condition. Chronic or persistent pain can sometimes be the after-effect of a recognised condition or injury, but remains after the original condition has resolved.
What has NICE said about acupuncture, CBT and ACT?
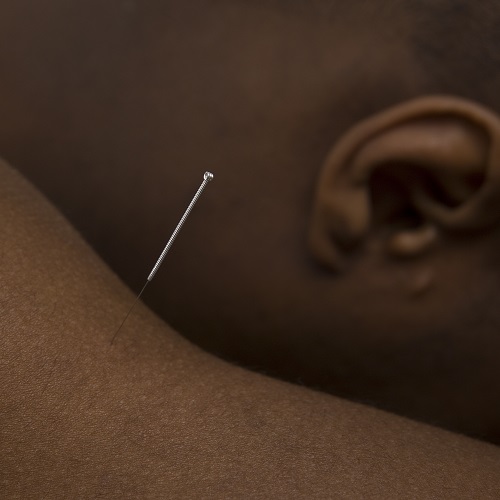
NICE has made clear the need to shift emphasis to putting the patient at the centre of care; and in particular the necessity that using opioid-based painkillers as a front-line treatment must decrease, with non-drug interventions taking more of a front-line role.
NICE found very little evidence to support using commonly-prescribed painkillers, instead prioritising exercise programmes (cardio, mind-body or a combination), talking therapies (CBT or Acceptance and Commitment Therapy), and acupuncture, along with and some types of antidepressants for the new draft guidelines.
What was the evidence for these three approaches?
Acupuncture (traditional or medical) for chronic primary pain: 27 studies examined by NICE, showed effectiveness of acupuncture, cost-effectiveness, and robust evidence for these.
CBT (Cognitive Behavioural Therapy) for chronic primary pain: CBT was seen to increase quality of life in patients with this condition, and was cost effective in doing so.
ACT (Acceptance and Commitment Therapy) for chronic primary pain: ACT was seen from research appraised by NICE, to improve sleep, quality of life and reduce pain and psychological distress, and was cost effective, therefore a good cost-benefit balance.
What will happen next?

The NICE draft guidelines are open to consultation up to the middle of September, following this the formal set of guidelines will be circulated to doctors and decision makers in the NHS.
When a doctor is looking at a case of a patient who is suffering with chronic primary pain, they will consider the patient in context, and which approach, or combination of approached is the the most suitable and fitting for the person. With the new draft guidance, it appears that CBT, ACT and acupuncture may become more commonly used in this area by the NHS.
In the meantime, this is a promising development in that the patient-centred methodology is beneficial for patients and their families, and the furthering of the model of a whole-person approach to care.
How do I access these services?
NICE recommendation doesn’t always mean NHS funding for all services, and the final guidelines affect how these are resourced, depending on cost, availability and so on, so this remains to be seen.
In the meantime, the above are all provided here at BCR privately, so if they wish to, patients can self-fund, or approach their healthcare insurer if applicable. In some cases certain healthcare charities also help toward the cost of private health services.
Resources:
NICE article on this subject from 03/08/2020: https://www.nice.org.uk/news/article/commonly-used-treatments-for-chronic-pain-can-do-more-harm-than-good-and-should-not-be-used-says-nice-in-draft-guidance
NICE draft for consultation: https://www.nice.org.uk/guidance/GID-NG10069/documents/draft-guideline

